Please note Dan’s story talks about child bereavement which some people may find triggering.
It all started in 2011. My Wife Jo and I found out that we were having naturally conceived triplets. The chances of conceiving triplets naturally are 1 in 10,000, and we were ecstatic! However, this is where it all started. From day one we had the control taken away from us. Nothing would be simple anymore. The Journey we was about to embark on would be one of fear, enjoyment, disbelief and heartbreak.
At 23 weeks Jo started to have complications which resulted in her having to have a suture (cervical stitch) to help her to progress with the pregnancy for as long as possible, this was to prove to be an ordeal. Three weeks later Jo started complaining of stomach pains and had a show (which I now know is a sign of labour!). We made our way up to the hospital. Jo was put into a room. A doctor came around and asked if she could just do a quick examination. Now, I am no doctor but I am pretty sure that the phrases I can feel a head and 8cms dilated are not words consistent with someone who is not in labour! And indeed I was right, this was it, Jo was in full on labour at 26 weeks. What happened next was a flurry of activity, panic and rushed phone calls! The hospital we were at was not equipped to take premature babies that early and our next nearest hospital had no beds available. It looked like we were going to Liverpool, or there were even talks of helicopters and Ireland. Finally right at the last minute the hospital near to us managed to free up three beds, an ambulance was called and Jo was put backwards on a trolley with her legs over her head and rushed off to the ambulance. I followed in the car as closely as I could whilst the ambulance, sirens, lights and all rushed Jo off to hospital.
When we arrived we were put into a private room and Jo was wired up to multiple machines, checking all three boys as well as Jo. She was given more drugs to slow down labour and steroids to help the boys tiny lungs to quickly develop. At this point everything seemed to be slowing down and a moment of relief and calm started. Jo’s mum was sent home and we settled down for a potentially long few days. Around 15 minutes later a doctor came into the room to check Jo and to come up with a plan of action. The doctor examined Jo. I could see immediately from his face that it was not the news we were hoping for. He explained that Jo’s waters were crowning and labour was going to happen. He then disappeared outside to call his consultant. When he returned he explained that the plan was to break the waters and to try to deliver George who was clearly adamant he was coming out. They would attempt to leave Charlie and Harry inside as they were identical and in the same sac and could potentially go on to reach term. We then received visits from multiple professionals including the NICU Team, doctors, and anaesthetists to explain what would happen next. There was so much information being thrown at us I don’t think I took any of it in. It was almost like I was a spectator and not really attached to the situation. I felt numb and completely overwhelmed with fear, anticipation and adrenaline.
I just remember looking at Jo and then the room, full of people and equipment. All ready to help to give our babies a chance at life. There were 3 professionals for each baby, and multiple professionals for Jo. And then it was time to start pushing. They broke Jo’s waters and she began delivery of George. I have no idea how long this went on for as we lost all sense of time. The next thing I remember was a nurse saying they could no longer find George’s heartbeat. What happened then was something I honestly thought only happened in really cheesy episodes of casualty. Every plug which was attached to Jo, the bed or equipment was literally yanked out of the wall, and doctors set off running down the corridor with Jo. Pushing incubators for the babies and all of the equipment along with them. They were all shouting orders to each and talking about an emergency C-Section. I was running down the corridor alongside Jo holding her hand until we came to a big set of double doors, I gave her a kiss and she was gone. I was left stood on my own in the corridor, just catching a final glimpse of Jo as the doors closed. It was silent. I had no idea what was happening in that room. The next thing I knew a neonatal nurse came to see me and asked would I like to quickly see my boys before they took them to intensive care. This was the first time anyone had spoken to me. This was the first time anyone had told me my boys had been born and were alive. I just remember asking how Jo was and she said Jo is OK. The nurse took me into the room where my boys were. And there they were, my three boys, Charlie, Harry and George. Covered from head to toe in wires, breathing apparatus and all inside zip lock bags with just their heads out to keep them warm. I can’t begin to explain what it was like to see them like that. I don’t think my brain would allow to me process it at that time. But they were here, and alive. After no more than two minutes my time was up. I was asked to go back to the room where Jo had been earlier and wait whilst the boys was rushed to intensive care and Jo was brought round from surgery.
Charlie, Harry & George had been born at 12.30am by emergency C- Section on the 03 July 2011. Charlie weighed 1lb 6oz, Harry 1lb 12oz and George only 1lb.
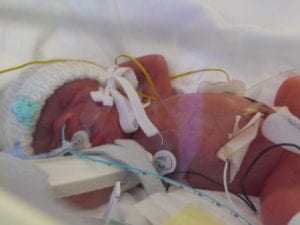
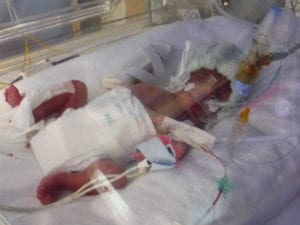
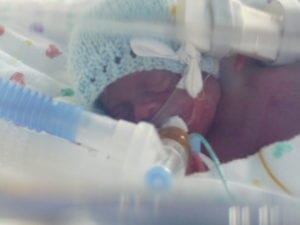
The first ten day’s were a blur. Hours after giving birth Jo got to meet her boys for the first time. Unfortunately she developed an an infection which meant she could not go to the NICU for five days. This was absolutely heart breaking. After five days Jo was over the worst and able to see her boys. However, my work had insisted that I return and so even this was bitter-sweet. I spent the following five nights sleeping at the hospital and going to work from there Until after 10 days Jo was allowed home.
The next few weeks were a rollercoaster. In a matter of just hours the boys would go from doing amazingly well to being in a critical. We went through multiple blood transfusions, infections, bradycardias, de-saturations, collapsed lungs and surgeries. It is amazing how quickly you pick things up you feel like a nurse not a parent. You have an immense feeling of not being in control, of hopelessness. You spend hours watching your children through a plastic box fighting to survive.

At 5 weeks old Harry got a serious infection of the gut known as Necrotizing Enterocolitis (NEC). We were Harry’s infection couldn’t be controlled by antibiotics and he would need surgery to examine the extent of the infection. We left the hospital because we couldn’t bear to sit watching the clock in the parents room. But we received a phone call shortly after asking us to return to the hospital as quickly as possible. We knew that this was not good news. We arrived back and were put into a side room where a nurse and the surgeon were waiting. They explained that the infection had destroyed all but 5cm of Harry’s gut and that there was nothing they would be able to do for him. They explained that there were two options. Stitch up his wound and see how long he survives on the ward, or to withdraw his care. We had to make the hardest decision of our lives and we decided that the only thing to do would be to withdraw Harry’s care and not to let him suffer any more pain. Harry was brought back up to the ward and we spent a little bit of time with him there. Because Harry had been so poorly, I had not been able to hold him. The first time I was able to hold my son was as I carried him to the Snow Drop suite where we would spend his final hours together. Harry died in my arms on the night of the 09/08/2011 at 11.57pm at 5 weeks old.

Just a day later we were back at the hospital for Charlie and George. Everything was so raw and yet we were back in the same room looking at an empty space where Harry had been the night before.
Charlie and George continued to get stronger, but it was not without its setbacks. They both still regularly got infections. Charlie had suspected NEC which thankfully was treated with the use of antibiotics. Charlie also had two collapsed lungs and had to be put back onto the ventilator for a short while. George’s eyes had not fully developed and so he had to have surgery. They kept fighting and getting stronger. After three months they were well enough to be moved to our local hospital. We had to stay strong for the final stretch.
After only a couple of weeks the boys were finally allowed home. George still only weighed 3lb and Charlie 4lb. If I thought hospital had been scary, having the boys home with no monitoring equipment or doctor was even scarier. It took a lot of getting used to! We had anxieties about people visiting them because of infection. We were terrified to take them out in case anyone so much as breathed on them, and this has taken us years to get over (and we are probably not even over it now really!)

The boys have continued to grow stronger and stronger. Today, George has suspected mild cerebral palsy which has only highlighted itself over the past year. Charlie has spastic paraplegic cerebral palsy which affects his lower legs meaning he is fully dependent on a wheelchair. Charlie is such a funny determined young man and George, such a caring and kind boy. They continue to make us very proud every day.
We went on to have two more children Tommy who is 3 and Hettie who is 6 months old and who are both just as fabulous.
It’s true that time does help with grief and trauma but we will always wonder what Harry would have grown up to be like, and that will never change.

Please see the links below for more support with any of the things Dan has discussed:
Spoons Dads Facebook Support Group
SANDS – Stillbirth and Neonatal Death Support
Join Spoons Dads Focus Group – shaping the support we offer NICU Dads